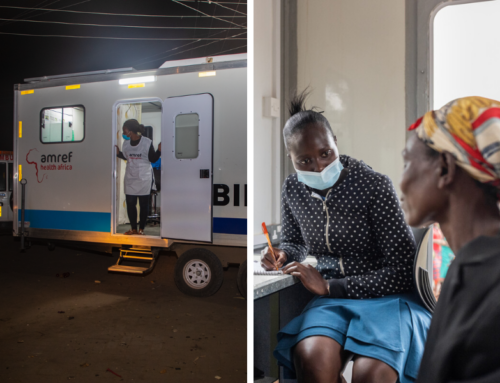
Investment in Africa’s health systems is vital if the continent is to achieve inclusive and sustainable growth.
According to the World Bank, Africa’s population is estimated to reach 2.5 billion by 2050. The region will face a critical challenge of creating the foundations for long-term inclusive growth.
At the moment, many African countries still contend with high levels of child and maternal mortality, and most health systems are not able to deal effectively with epidemics and the growing burden of chronic diseases, such as diabetes.
These challenges call for accelerated progress toward embracing universal health coverage (UHC), whose principle is that everyone receive needed health services without financial hardship.
The World Health Organization has set aside 12th December as UHC Day to commemorate the anniversary of the first unanimous United Nations resolution calling for countries to provide affordable, quality health care to every person, everywhere.
UHC has been included in the new global Sustainable Development Goals (SDGs) adopted unanimously by member states of the United Nations. Most African countries have integrated UHC as a goal in their national health strategies.
However, the progress in translating these commitments into expanded domestic resource allocation for health, and ultimately, equitable, quality health services and increased financial protection has been far too slow.
To achieve their UHC targets by 2030, countries will need to eliminate preventable maternal and child deaths, strengthen resilience to public health emergencies, reduce financial hardship linked to illness, and strengthen the foundations for long-term economic growth.
Africa has made some progress in reducing child deaths. According to the World Bank, at least 12 out of 20 sub-Saharan African countries for which recent data is available have experienced a decline of at least 4.4 per cent per year in infant and under-5 mortality rates between 1990 and 2015. A case in point is Kenya, which has also recorded a similar improvement in maternal health.
Through the free maternity services programme, for example, Kenya has doubled deliveries in health facilities from 600,323 in 2013 to 1.2 million in 2016 and increased primary health care use from 69 per cent in the financial year 2013/2014 to 77 per cent in 2015/2016 as a result of foregone user fees.
But, realising universal health coverage, and the health-related SDGs, will not be possible without community health workers becoming an integral part of sufficiently resourced health systems. Community health workers close the gap between communities and the formal health system.
They have a very important role in referral, health promotion and prevention at the community level. Their effective involvement leads to significantly better health outcomes. Community health workers provide health education and referrals for a wide range of services, and provide support and assistance to communities, families and individuals with preventive health measures and in gaining access to appropriate curative health and social services.
Another prerequisite for achieving UHC is to substantially increase health financing and the recruitment, development, training and retention of the health workforce – especially in developing countries. This is covered under target 3c of the global Sustainable Development Goals.
The vision of WHO’s Workforce 2030 report is that by 2030 all communities should have access to trained and supported health workers with a minimum core set of competencies.
Non-Governmental Organizations (NGOs), such as Amref Health Africa, a leading NGO in this area, are working to fill the gaps in the lack of affordable, quality health care in disadvantaged or remote African communities.
As Amref Health Africa, we work with a network of community health workers spread across Africa and have observed that the community places a tremendous amount of trust in them to convey accurate information about health and health care.
Our focus on community-based health solutions is informed by the gap we have identified between vulnerable communities and the rest of the health system. These communities are often, but not always, remote geographically, but they are very remote in practical terms from policy makers and health system managers.
There is an urgent need for community health workers to be recognised as key players within communities in addressing health issues. Current high attrition rates for community health workers pose a serious threat for people accessing health services. The attrition rate varies, but is often up to 77% per year.
Without proper policies in place, the attrition rate will continue to escalate. Remuneration is a key factor in addressing attrition of community health workers as it gives income stability and commitment to work.
African governments must increase the funding available for health so that they are able to provide essential health care services of sufficient quality. Every country should mobilise additional domestic resources for health and diversify its funding sources.
Africa’s health systems must meet the needs of the most vulnerable; they must place people at the centre and ensure wider use of indigenous knowledge, and promote enlightened leadership if we are to achieve universal health coverage and other sustainable development goals related to health.