 Canada-Africa Initiative to Address Maternal, Newborn and Child Mortality
Canada-Africa Initiative to Address Maternal, Newborn and Child Mortality
Project Timeline: March 2016 to March 2020
Funders: Government of Canada through Global Affairs Canada, individual Canadians, businesses and foundations.
Results Highlights:
- CAIA-MNCM: Impact Overview All Countries
- CAIA-MNCM: Ethiopia Impact Overview
- CAIA-MNCM: Kenya Impact Overview
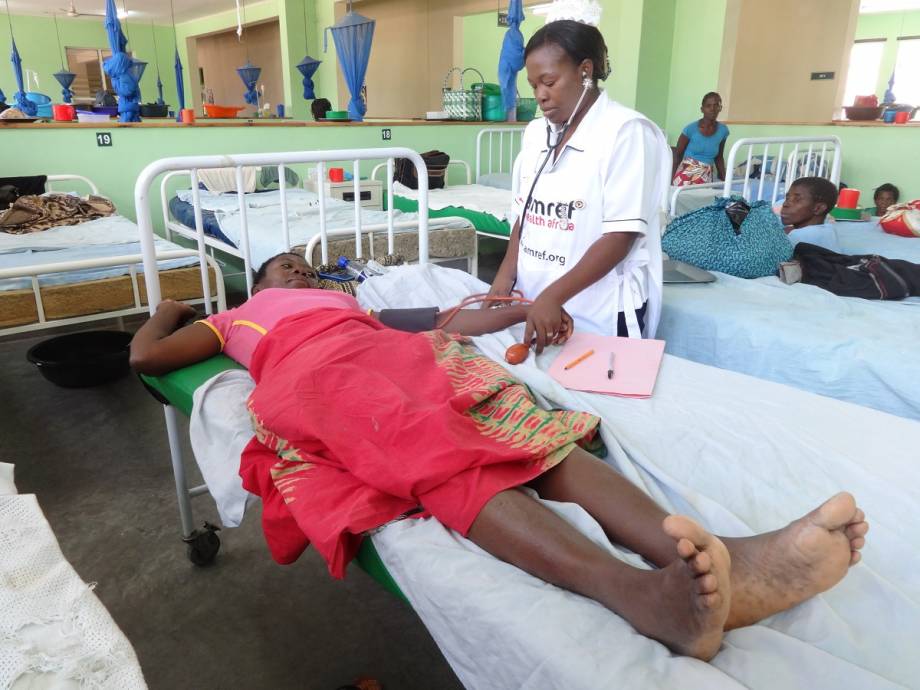
- CAIA-MNCM: Malawi Impact Overview
- CAIA-MNCM: Tanzania Impact Overview
- CAIA-MNCM: Senegal Impact Overview
Situation: Rural and remote areas lacked access to basic health care essential for mother and child survival
Significant progress has been made around the world in reducing the number of women who die in pregnancy or childbirth – the rate dropped globally by 43% between 2000 and 2015. Yet, in many communities in sub-Saharan Africa, the maternal and newborn mortality rates continue to be unacceptably high.
- 550 women in sub-Saharan Africa continue to die every day from complications related to pregnancy and childbirth (compared to 5 in developed countries).
- 985,000 newborns in Africa died in 2015 alone.
Mothers and newborns in remote, rural and fragile communities are at greatest risk because they lack access to basic, life-saving health care and everyday infrastructure, such as clean water and sanitation, so important for healthy living.
Action: Worked in partnership to reduce mother and newborn deaths in rural or remote areas
We brought together Canadian and African expertise to tackle key contributors to poor health, including:
- poor access to family planning and other sexual and reproductive health services;
- lack of clean water;
- inadequate sanitation;
- shortage of trained health workers;
- gaps in information for parents about basic child health;
- malnutrition and under nutrition;
- overcrowded and poorly equipped health facilities;
- lack of systems to track vital health data; and,
- gender inequality
Partners
Project Results: Highlights
- 3,316,154 people reached through health-focused activities in 20 communities in Ethiopia, Kenya, Malawi and Tanzania
- 664,813 people informed about better health practices at home and in their community
- 37,986 copies of educational materials on nutrition provided to parents, volunteer community health workers and teenagers
- 1,047 volunteer Community Health Workers trained to provide basic health education and services for families
- 2,422 health workers trained to improve their skills in areas such as family planning, emergency care for pregnant women and nutrition
- 543 women screened for gynaecological conditions, such as cervical cancer and obstetric fistula
- 95 health workers trained on providing teenagers with youth-friendly health care services
- 44 health facilities upgraded, including building new maternity wards and labour rooms
Community Voices

Mearem Dawud, midwifery student, Ethiopia
In the Afar region of Ethiopia, the project supported 16 young women to attend a three-year training program to become midwives. Mearem Dawud is one of the students.
Afar is a rural area with pastoralist (nomadic) communities. In these types of areas, well-trained midwives are essential for ensuring women have access to quality health care during pregnancy and delivery.
“Afari girls are afraid of getting health services, because there is a lack of female health workers and because they are afraid of taking health services in the presence of males. Also, many girls have gone through Female Genital Mutilation [FGM, also known as Female Genital Cutting or FGC] and thus they become afraid of going for health services. So, I am hopeful that I can help girls by providing health services myself. I am also hopeful that I can help to change attitudes in my community on harmful traditional practices [such as FGM/C] by facilitating dialogue in my community.”
— Mearem Dawud

